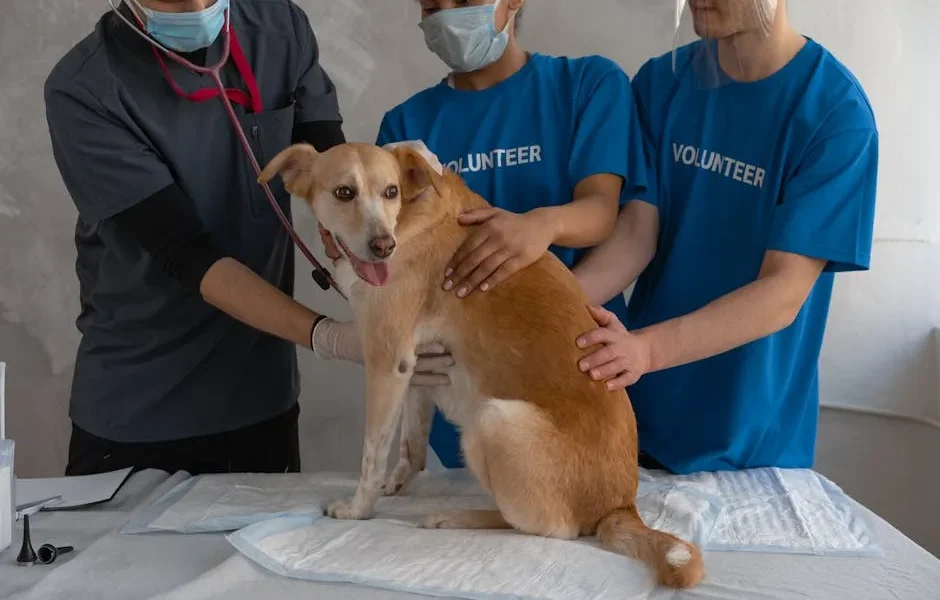
- Managing chronic illness in pets means working closely with your vet. You’re not just following orders.
- Set up home care routines and track symptoms. This helps treat diabetes, kidney disease, and arthritis better.
- Talk to your vet regularly. Be honest about what works and what doesn’t. This helps adjust care as your pet’s needs change.
I still remember when my cat Oliver got diabetes. He was only seven years old. Suddenly we needed twice-daily insulin shots, special food, and glucose tests.
My vet gave me papers and said something important: “You’re not just following my orders anymore. You’re part of Oliver’s medical team now.”
That changed everything. Chronic Illness Management in Pets: How to Partner with Your Vet for Long-Term Care is about this partnership.
You won’t become your pet’s doctor. That’s not your job. But managing a chronic condition takes time. It’s a marathon, not a sprint. And you’ll be there every single day.
When Life Becomes Long-Term Care
Here’s a surprise for most pet parents: about 60% of dogs over age ten have at least one chronic condition. So do 40% of cats over ten.
We’re not talking about quick antibiotics. We mean arthritis, kidney disease, diabetes, heart problems, thyroid issues. These don’t go away. But they can be managed.
Why are we seeing more chronic illness? Our pets live longer now. Average dog lifespan jumped from 10.5 to 11.8 years over the past twenty years.
That’s wonderful news. But it means we face things earlier pet owners rarely saw.
Let’s be honest. Nobody prepares you for this. You bring home a puppy or kitten. You think about vaccinations and maybe spaying or neutering.
You don’t imagine giving injections. Or calculating medication doses. Or learning to read symptom patterns.
Building Your Medical Partnership
What does real partnership look like? You and your vet bring different things.
Your vet has medical training. They have diagnostic tools and treatment protocols.
But you have something equally valuable. You see your pet daily. You recognize patterns. You know what’s normal for your pet.
The Art of the Vet Visit
I learned quickly with Oliver to come prepared. Not just with questions. But with data.
How much water is your pet drinking? Any changes in appetite, energy, or behavior? Good days and bad days, or consistent?
Studies show only 50-70% of pet owners give chronic medications correctly. That’s a problem. But here’s the thing: sometimes it’s not about following directions. It’s about communication.
If you struggle to give a pill, tell your vet. If the schedule doesn’t fit your work routine, speak up.
There are almost always alternatives. Different forms. Compounded medications with flavoring. Transdermal options.
Your vet can’t solve problems they don’t know about.
I keep a running note on my phone. Weird things I notice. Questions that pop up at 2 AM when I’m worrying.
By appointment day, I have concrete information. Not vague concerns.
I’ve learned to ask: “What should I watch for at home?” and “What would make me call you before our next visit?”
When to Loop in Specialists
Your primary vet is your quarterback. But sometimes you need specialty players.
For complex conditions, specialists help. Advanced kidney disease. Poorly controlled diabetes. Cancer. They bring focused expertise.
The key is coordination.
Many vet practices now share digital records. Your primary vet, specialists, and vet technicians work together on your pet’s care plan.
Ask about this. Make sure everyone’s on the same page. You shouldn’t be the sole go-between for different providers.
Creating Your Home Care System
Here’s where partnership gets practical. Managing chronic illness means routines that work for both you and your pet.
It sounds simple. But it’s where most people struggle.
For Oliver’s diabetes, I needed to give insulin exactly twelve hours apart. Sounds easy. Until you factor in work schedules. Social plans. Travel.
I had to get creative. And honest with myself about what I could actually maintain long-term.
Because chronic means ongoing. Not for a week or a month. But potentially for years.
The Power of Tracking
You know what made the biggest difference for Oliver? A simple tracking system.
I used a basic app at first. Just logging insulin doses and meal times. Then I started adding notes. Seemed sluggish today. Drank more water than usual. Had the zoomies at 3 PM.
Those patterns became invaluable. When we needed to adjust his insulin, my vet had weeks of data. It showed exactly how Oliver responded to different amounts.
We weren’t guessing. We were making informed decisions.
For pets with arthritis (about 20% of adult dogs), tracking good versus painful days helps. You see if pain management is working.
For senior cats with kidney disease (30-40% of them), noting water intake and litter box habits gives early warning. You catch problems before they get worse.
Medication Realities
Let’s talk about the hard part: giving medications consistently is tough.
Pills get skipped. Doses get doubled because you can’t remember if you already gave the morning one. Liquid medications get refused.
I’ve learned a few tricks. Pill pockets work until they don’t. Then you need a new strategy.
For Oliver, I crushed his thyroid medication (after checking with my vet that this was okay). Mixed it with a tiny amount of tuna juice. Worked far better than fighting him twice daily.
Some pets do better with compounded medications in different forms. It might cost a bit more. But if it means you’ll actually be able to give it reliably? Worth every penny.
There’s also growing availability of flavored medications for pets. Chicken-flavored antibiotics. Tuna-flavored kidney support supplements.
The point is: don’t suffer in silence. If medication is a battle, tell your vet. They need this information to help you find solutions.
The Financial Reality Check
We need to talk about money. Chronic illness management can cost $200 to $6,000+ per year. It depends on the condition.
That’s not nothing.
I’ve found that honest conversations with your vet about budget don’t make you a bad pet parent. They make you a realistic one.
Most vets would rather help you prioritize what’s essential. Better than watching you silently struggle. Or worse, just stop treatment altogether.
Ask about generic medication options. Ask if certain diagnostic tests can be spaced out differently if your pet is stable. Understand which treatments are “nice to have” versus “must do.”
Some practices offer payment plans for chronic care. Pet insurance can help if you have it before diagnosis. Though many policies limit chronic conditions.
CareCredit and similar medical credit options exist for ongoing vet expenses.
Recognizing When Treatment Works (and When It Doesn’t)
How do you know if management is working? This is tricky.
Improvement with chronic disease often means “staying stable” rather than “getting better.”
For Oliver’s diabetes, success looked like consistent blood glucose in an acceptable range. For a dog with arthritis, it might mean being willing to go for walks again. Or navigating stairs more comfortably.
For cats with kidney disease, stable kidney values and good appetite signal effective management.
But here’s what I wish someone had told me: if your pet’s quality of life isn’t what you’d hoped for, that’s worth discussing.
Maybe the treatment needs adjusting. Maybe there are additional therapies to try. Or maybe your expectations need adjusting to what’s realistic for that condition.
Vets report that proper chronic disease management can extend quality life by 2-5 years on average. For most conditions.
Quality is the key word. More time isn’t always better if that time is spent suffering.
The Quality of Life Conversation
This is the hardest part of chronic illness management. So I’ll be direct.
You need to revisit quality of life assessments regularly. Not just at crisis points. As an ongoing part of your partnership with your vet.
Many practices now use quality of life scales. Objective measures of appetite, mobility, pain levels, and engagement with family.
These tools help remove some emotion from what’s inherently emotional. You’re not being pessimistic by bringing this up. You’re being a responsible advocate for your pet.
When Technology Helps
Chronic illness management has changed dramatically in just the past couple years.
Telemedicine options mean you can do check-ins for stable conditions without clinic stress. For anxious cats or dogs with mobility issues, this is huge.
Wearable technology and activity trackers are increasingly used. Some diabetes management now involves continuous glucose monitors. Similar to what humans use.
Heart disease patients might have activity monitors. They track changes in exercise tolerance.
Even simple fit bits for pets can reveal patterns. Rest versus active time informs arthritis management.
Is all this necessary? Not always. But ask your vet what technologies might help your pet’s specific condition.
Sometimes a $50 activity tracker provides information worth hundreds in diagnostic testing.
The Communication Loop
Here’s something I’ve learned after years of managing Oliver’s multiple conditions: good communication isn’t just about talking.
It’s about creating systems that work even when things are routine.
I have scheduled check-ins with my vet every three months for Oliver. Even if he seems fine. We review his tracking data. Adjust medications if needed. Discuss any subtle changes.
This proactive approach has caught problems early more than once. Before they became emergencies requiring emergency veterinary care.
Between appointments, I know exactly when to call. If Oliver misses more than one meal. If I see any specific warning signs we’ve discussed. Or if my gut just says something’s off.
Trust your instincts on that last one. You know your pet better than anyone.
But also? Know when NOT to panic. Some fluctuation is normal with chronic conditions.
Understanding your pet’s normal behavioral patterns helps you tell the difference. Between “call right now” and “make a note to mention at next appointment.”
Finding Your Rhythm
Multi-modal management combines medication, diet changes, and lifestyle changes. It’s standard for most chronic conditions.
About 65% of cases require medication. 80% benefit from dietary adjustments. 70% need lifestyle modifications.
That’s a lot of plates to keep spinning.
The truth? You’ll probably mess up sometimes. You’ll forget a dose. Or give the wrong medication. Or miss a subtle sign that something’s changing.
I certainly have. What matters is the overall trend. The consistent effort. The willingness to adjust when something isn’t working.
Oliver lived three more good years after his diabetes diagnosis. Years I wouldn’t have had if I’d been too intimidated to become an active partner in his care.
Were those years perfect? No. Did I sometimes resent the rigid schedule and expense and worry? Absolutely.
But I also got three more years of him curling up on my lap and purring. That partnership with my vet made those years possible.
Final Thoughts
Managing chronic illness in pets isn’t about becoming a vet expert. Or doing everything perfectly.
It’s about showing up consistently. Communicating honestly. And recognizing that you’re the constant in your pet’s life.
Your veterinary team provides the medical expertise. Together, that partnership creates the best possible outcomes.
These conditions can’t be cured. But they can absolutely be managed.
If you’re just starting this journey, take a breath. It feels overwhelming at first. But you’ll find your rhythm.
Schedule that next appointment. Ask those questions you’ve been wondering about. Start that tracking system, even if it’s just notes in your phone.
And remember: choosing the right veterinary partner who communicates clearly makes all the difference. One who respects your role in your pet’s care.
You’ve got this. And more importantly, you’re not doing it alone.
Sources & Further Reading
- American Veterinary Medical Association — Comprehensive pet health resources and guidelines for chronic disease management
- American Animal Hospital Association — Evidence-based pet care recommendations including senior pet wellness guidelines
- American College of Veterinary Internal Medicine — Specialty care information for chronic and complex medical conditions
- Veterinary Information Network — Professional veterinary resource with pet owner education sections