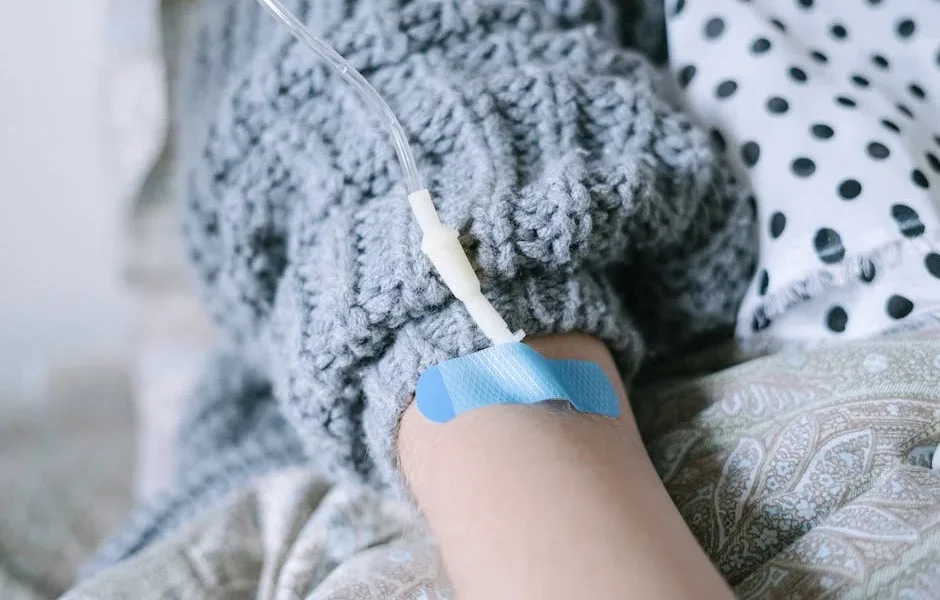
- Pets have far fewer side effects from chemo than humans. Only 20-30% have bad reactions. Treatment focuses on quality of life, not aggressive elimination.
- Chemo for pets like dogs with lymphoma works well. 80-90% go into remission. They live 12-14 months instead of just 4-6 weeks without treatment.
- Treatment costs $3,000-$10,000 for complete protocols. But financial help and payment plans are available through many clinics and nonprofits.
I’ll never forget Mrs. Patterson’s face when I told her Cooper had lymphoma. Her Golden Retriever was only seven. He was full of life just weeks before.
But what surprised her most? When I explained that Chemotherapy for Pets: Treatment Options & What to Expect 2025 looks very different from human cancer treatment.
Cooper wouldn’t lose his beautiful coat. He wouldn’t spend days vomiting. He’d likely play fetch the same afternoon as his treatment.
That conversation happens in our clinic almost weekly now. Cancer diagnoses in pets are increasing. Owners are understandably terrified.
But here’s what most people don’t realize: Pet chemo is designed around a completely different philosophy than human cancer treatment.
Why Chemotherapy for Pets Matters More Than Ever
The veterinary cancer field has changed dramatically over the past decade. We’re not just extending survival times anymore. We’re giving pets genuinely good months or even years with their families.
The numbers tell a compelling story. Dogs with lymphoma have only 4-6 weeks without treatment. That’s one of the most common cancers we see.
With chemotherapy? That jumps to 12-14 months of quality time. That’s birthday parties, holiday photos, beach trips, and lazy Sunday mornings.
And unlike human chemo, we use about 25-30% lower doses. Our goal isn’t remission at any cost. It’s extending good days while minimizing bad ones.
The Side Effect Reality Check
When you picture chemo, you probably imagine hair loss and constant nausea. You might think of weekends spent in bed.
Here’s the truth for pets: only 20-30% have significant side effects. Most dogs and cats continue their normal routines. They eat. They play. They don’t understand they’re sick.
Cats generally handle chemo even better than dogs. Their calm nature means less gastrointestinal upset. Their lower activity levels make fatigue less noticeable.
Step 1: Get a Proper Diagnosis and Staging
Before any treatment discussion happens, we need to know exactly what we’re dealing with. This isn’t the time to skip diagnostic steps or cut corners on testing.
Your veterinarian will likely recommend:
- Biopsy or cytology to confirm cancer type and grade
- Blood work including complete blood count and organ function panels
- Imaging such as X-rays, ultrasound, or CT scans to determine spread
- Staging tests specific to cancer type (bone marrow tests for lymphoma, chest X-rays for metastasis checks)
Staging determines how advanced the cancer is. A Stage I lymphoma in one lymph node is different from Stage V with bone marrow involvement.
This information directly impacts whether chemo makes sense for your pet.
When to See a Veterinary Oncologist
Most general vets will refer you to a specialist for chemo. Board-certified veterinary oncologists have advanced training in cancer treatment.
They have access to protocols your regular vet might not offer.
That first oncology visit typically costs $200-$400. It includes a thorough exam, treatment plan discussion, and prognosis conversation.
Don’t skip this step. The specialist might identify options your regular vet doesn’t have. This could include clinical trials or newer targeted therapies.
Step 2: Understand Your Treatment Protocol Options
Not all chemo looks the same. The protocol your oncologist recommends depends on several things. These include cancer type, stage, your pet’s overall health, and your family’s goals.
Multi-Drug Combination Protocols
For aggressive cancers like lymphoma, combination chemo is standard. This means using multiple drugs in rotation.
The CHOP protocol is the gold standard for dog lymphoma. It uses Cyclophosphamide, Hydroxydaunorubicin (doxorubicin), Oncovin (vincristine), and Prednisone.
These protocols typically run 12-24 weeks. Treatments happen every 1-3 weeks.
Yes, it’s a time commitment. But most sessions take just 30-60 minutes. Many pets can be dropped off in the morning and picked up later.
Single-Agent Chemotherapy
Some cancers respond well to individual drugs. Mast cell tumors might receive Palladia or lomustine as single agents.
Bladder cancer often responds to Piroxicam combined with mitoxantrone.
Single-agent protocols are simpler. They’re often more affordable. Sometimes your regular vet can give them instead of requiring oncology visits.
Metronomic Chemotherapy
This newer approach uses low-dose oral chemo given continuously at home. Instead of high peaks and valleys, it provides steady, gentle tumor suppression.
It causes minimal side effects.
Research from 2024 shows particular promise for mast cell tumors. It also works as maintenance therapy after remission with traditional protocols.
It’s not right for every cancer. But it’s worth discussing with your oncologist.
Targeted Therapies and Immunotherapy
The landscape changed in 2024. The FDA approved monoclonal antibody treatments for dog B-cell lymphoma.
These drugs specifically target cancer cells. They leave healthy tissue alone. This results in fewer side effects than traditional chemo.
Tyrosine kinase inhibitors like Palladia block signals that cancer cells need to grow. They’re pills given at home. This makes them convenient for owners who can’t manage frequent clinic visits.
Step 3: Prepare Your Home and Family
Once you’ve committed to treatment, some practical preparations make the process smoother.
Safety Precautions
Chemo drugs are excreted in your pet’s urine, feces, vomit, and saliva. This happens for 48-72 hours after treatment.
This means precautions:
- Wear disposable gloves when cleaning litter boxes or picking up waste
- Double-bag pet waste and seal before disposing
- Wash any bedding or towels separately from family laundry
- Pregnant women and immunocompromised family members should avoid handling waste entirely
- Keep pets away from areas where children play during the 72-hour window
Sounds intimidating? It becomes routine quickly. Most families adapt within the first treatment cycle.
Medication Organization
Your pet will likely get several medications. These include anti-nausea drugs, antibiotics if white blood cell counts drop, appetite stimulants, and possibly pain management.
I recommend a simple chart on your refrigerator. Track what gets given when.
Set phone reminders. Seriously. It’s easy to forget the evening anti-nausea pill when you’re juggling work, kids, and worry.
Step 4: Monitor and Manage Side Effects at Home
Side effects are less common and severe in pets. But they still happen. Knowing what to watch for and when to call makes all the difference.
Common Side Effects to Expect
Mild gastrointestinal upset tops the list. Some pets have decreased appetite, mild vomiting, or soft stool. These usually resolve within 24-48 hours.
Lethargy might occur for a day or two after treatment. If your normally energetic dog wants to nap more, that’s okay.
But if they won’t get up for meals or potty breaks, call your vet.
Low white blood cell counts are the most serious concern. Neutropenia (low neutrophil count) typically occurs 7-10 days after certain chemo drugs.
Your oncologist will schedule blood work to monitor this. Signs include fever, lethargy, loss of appetite, or any sign of infection.
When to Call Your Veterinarian Immediately
Don’t wait if your pet shows:
- Temperature above 103°F (normal is 100-102.5°F)
- Vomiting or diarrhea more than 2-3 times in 24 hours
- Complete loss of appetite for more than 24 hours
- Extreme lethargy or weakness
- Difficulty breathing
- Blood in vomit or stool
These could indicate neutropenia with infection. This is a true emergency requiring immediate hospitalization.
Similar to how you’d handle severe allergic reactions, time matters with chemo complications.
Appetite Support Strategies
Some pets become picky eaters during treatment. Try warming food slightly to enhance aroma. Offer smaller meals more frequently. Add low-sodium chicken broth.
Appetite stimulants like mirtazapine or maropitant work wonders when needed.
One trick I share with clients: rotate through several different high-quality foods. What your pet refuses Monday might be appealing Wednesday.
Step 5: Plan for Financial Realities
Let’s address the elephant in the exam room. Chemo for pets costs money. Often significant money.
Typical Cost Breakdown
Full chemo protocols typically range $3,000-$10,000. This depends on:
- Cancer type and protocol complexity
- Pet size (larger dogs require more drug, thus higher cost)
- Geographic location (urban specialists cost more than rural clinics)
- Monitoring requirements (frequent blood work adds up)
- Individual drug prices (newer targeted therapies cost more than traditional chemo)
Individual chemo sessions run $150-$600. A CHOP protocol for lymphoma in a 60-pound dog might total $5,000-$7,000 over six months.
Compare this to major surgical procedures. Chemo costs are substantial but not necessarily higher than other life-saving treatments.
Financial Assistance Options
Don’t assume you can’t afford treatment without exploring options:
- Pet insurance: If your pet has coverage, cancer treatment is usually included. You’ll still have deductibles and copays. This is why we recommend insurance for young, healthy pets—before problems develop.
- CareCredit and veterinary financing: Interest-free periods (usually 6-12 months) help spread costs.
- Nonprofit assistance: Organizations like the Pet Fund, Brown Dog Foundation, and Magic Bullet Fund offer grants for specific cancers.
- Clinical trials: University veterinary hospitals often seek patients for research studies. These offer reduced-cost or free treatment.
- Payment plans: Many oncology practices offer in-house financing.
Making the Value Decision
Only you can decide if chemo fits your family’s financial and emotional situation.
Some factors to consider:
Is your pet’s prognosis measured in months or years? A 13-year-old dog with aggressive cancer and a 3-month prognosis is different from a 6-year-old with a 2-year prognosis.
What’s your pet’s quality of life currently? If they’re already struggling, chemo might not add good time. If they’re still vibrant and happy, treatment could preserve that.
Similar to other major veterinary decisions, there’s no single right answer.
Trust your knowledge of your pet and your family’s circumstances.
Step 6: Track Progress and Adjust as Needed
Chemo isn’t a set-it-and-forget-it treatment. Your oncologist will monitor response. They’ll adjust protocols based on how your pet responds.
Measuring Treatment Success
For many cancers, we measure tumor size at regular intervals. Lymph nodes shrinking, masses becoming smaller, or bloodwork normalizing all indicate response.
“Remission” in pet oncology means we can’t detect cancer anymore. It doesn’t mean cured. Microscopic disease often remains.
But remission can last months or years. This provides quality time.
“Stable disease” means cancer isn’t growing but hasn’t disappeared. Sometimes that’s the goal, particularly with slow-growing tumors.
Quality of Life Assessments
We use quality of life scales to objectively evaluate whether treatment is worthwhile. These tools assess appetite, mobility, pain levels, and overall happiness.
If quality of life declines despite treatment, it’s okay to stop. Truly.
Pet oncology success isn’t about pushing treatment at all costs. It’s about good days with your pet.
Common Mistakes to Avoid
Waiting too long to start treatment. Some cancers progress rapidly. That “let’s wait and see” approach can mean losing the window where treatment works best.
If your vet recommends urgency, listen.
Skipping follow-up blood work. Those recheck appointments aren’t optional cash grabs. They detect potentially life-threatening complications before your pet shows symptoms.
Neutropenia caught early is manageable. Neutropenia caught when your pet collapses is a crisis.
Stopping medication early because your pet “seems fine.” Chemo protocols are designed with specific timing and dosing. Skipping treatments or stopping early reduces effectiveness dramatically.
Not asking questions. Your oncologist expects questions. What’s the goal—remission or just buying time? What happens if we do nothing? What’s Plan B if this doesn’t work?
These aren’t rude questions. They’re essential conversations.
Comparing pet treatment to human treatment. Your friend’s experience with breast cancer chemo isn’t relevant to your dog’s lymphoma treatment.
Different doses, different goals, different side effects.
Forgetting to live. Yes, your pet has cancer. But they don’t know that. They want walks and treats and belly rubs.
Don’t let treatment consume every moment of the time you have left together.
Tips for Success Throughout Treatment
Build a support team. Besides your oncologist, maintain regular communication with your primary vet. They can often handle simpler needs like anti-nausea refills or sick visits between chemo appointments.
This saves you trips to the specialty hospital.
Similar to building a relationship with your regular vet, good communication with your oncology team makes everything easier.
Keep a treatment journal. Note what day chemo is given, which drugs, and how your pet responds over the following week.
Patterns emerge. Maybe your dog always feels punk on day 3 but rebounds by day 5. Knowing this reduces anxiety and helps you plan your schedule.
Ask about at-home options. More oral chemo medications are available now than ever before. If weekly trips to the oncologist are difficult, ask about home options.
Some portions of your pet’s protocol might be transitioned to home administration.
Connect with other pet cancer families. Online support groups and Facebook communities exist specifically for pet cancer. Sometimes talking with someone who’s been through it helps more than any vet explanation.
Celebrate small wins. Lymph nodes shrinking. Appetite returning. A good recheck bloodwork.
These victories matter. Take photos. Make memories. That’s what this is all about.
What About Alternative or Holistic Options?
Many owners ask about alternatives to chemo. They mention CBD oil, dietary changes, herbal supplements, or holistic approaches.
Here’s my honest take: I’m not opposed to complementary therapies that improve quality of life.
Acupuncture can help with pain and nausea. CBD might improve appetite and reduce anxiety. Omega-3 fatty acids have anti-inflammatory properties that might slow some tumor growth.
But—and this is critical—none of these replace chemo for cancers that respond well to conventional treatment.
Will mushroom supplements cure lymphoma? No. Could they support overall immune function alongside chemo? Possibly.
Always discuss supplements with your oncologist. Some interact with chemo drugs or interfere with treatment effectiveness.
Looking Ahead: New Developments in 2025
Pet oncology is evolving rapidly. Monoclonal antibodies approved in 2024 represent just the beginning of immunotherapy options.
These treatments harness your pet’s immune system to fight cancer. They often have fewer side effects than traditional chemo.
Artificial intelligence tools are beginning to help predict which patients will respond to which protocols. This potentially allows customized treatment from day one rather than trial and error.
Telehealth oncology consultations expanded dramatically after the pandemic. This makes specialist opinions accessible to pet owners in rural areas who previously had no options.
And research continues. University veterinary hospitals across the country need patients for clinical trials. These test new drugs and protocols.
These trials offer cutting-edge treatment often at reduced cost. They also advance veterinary medicine for future patients.
Final Thoughts
Cancer isn’t the death sentence it once was for pets. Modern chemo protocols can add months or years of genuinely good quality time. When appropriate for your pet’s situation.
Yes, it requires commitment. Financial, emotional, and logistical commitment.
But for many families, those extra holidays, birthdays, and ordinary Tuesday evenings together are priceless.
If